A Clean Cut: A Look Into Surgery for Table Saw Related Injuries
This is a sidebar to our exclusive feature on flesh-sensing technology and what it means to the remodeling industry. Click here to read the main story.
Many people wonder how likely it is that finger reattachment surgery will have a successful outcome. But that’s the wrong question to ask, says Dr. Jeffrey Wint, a spokesperson for the American Academy of Orthopedic Surgeons. Instead, the relevant statistic is how many replantations are attempted.
“Fingers reattached at a good facility are 80 to 90 percent successful, but that doesn’t include all of the people who are not candidates for the surgery,” says Wint, who is also a hand and orthopedic surgeon in Springfield, Mass. “If you’re a 55-year-old smoker with a single finger severed near the base, I’m probably not going to do that surgery.”
Indeed, one study conducted by the University of North Carolina, Chapel Hill, looked at every hospital admission for finger amputations statewide during 2004–2005. In a total of 556 cases, only 16 percent were able to receive replantations.
In addition, even when a digit is successfully reattached, all patients will have some loss of sensation. Many will also experience a diminished range of motion and increased sensitivity to cold.
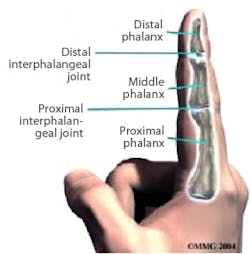
Generally, distal injuries—those at the fingertip or near the first knuckle—are simpler to repair. Conversely, proximal wounds, closer to the base of the finger, involve severed tendons and sometimes are an indicator not to replant. The width of the saw kerf is also important because a cleaner, narrower cut creates less tissue damage. The condition of the severed digit needs to be assessed as well, since without proper storage, it’s no longer viable after six hours.
Another variable lies in the number of fingers involved or whether multiple injuries have occurred on the same digit. This can lead to more creative solutions.
“If someone cuts off their index, middle, and ring finger, and the index is badly damaged, but the ring finger is OK, a surgeon might relocate the ring finger to the index position,” Wint explains.
Then there are the patients themselves. Age, general health, and whether he or she is a smoker are all important considerations, along with the level of disability presented by the finger’s absence. For example, reattachment surgery will almost always be attempted for a thumb.
The procedure itself, a four-to-five-hour microsurgery, is complex. Two teams are required—one for the recipient and one for the finger—and afterward the patient will need to recover in an intensive care unit, along with weeks, or even months, of rehabilitation.
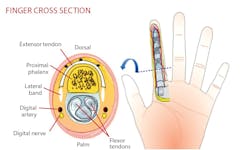
Before the replantation begins, the surgeon will identify and tag all relevant tendons, arteries, veins, and nerves. This is the final opportunity to ensure that every component is viable and that the blade’s path wasn’t too destructive for a successful outcome. The first section actually reattached is bone. It will need shortening, and in the case of a jagged break, the surgeon will shave both sides before inserting pins or wires or a combination of the two. Next, the tendon is sewn together. Then come arteries and veins, which are arguably the most challenging aspect of the procedure, requiring a 10X microscope.
Blood vessels are hollow and difficult to stitch, and veins in particular can easily collapse or tear. For every artery he sews, Wint makes it a practice to reattach two veins to ensure adequate blood flow as well as proper drainage. The final steps are the reattachment of nerves and skin.
“Even with a great prognosis, this is a serious thing,” Wint says. “My son is 23, and I keep my power saw hidden so that he has to ask for it. It takes less than 60 milliseconds for the blade to cut through a human forearm.”
About the Author
Erika Mosse
Director of Content
Erika Mosse is the former director of content for Professional Remodeler.